Abscesses in Pets: Types, Warning Signs, and Treatment
Your cat is limping and has a soft, warm swelling on their leg that wasn’t there yesterday. Your dog’s face looks different on one side, with a swelling that appeared below the eye seemingly overnight. An abscess has a way of producing signs that feel both alarming and hard to interpret, partly because the word covers a wide range of presentations in different locations and from different causes. Knowing the most common types, what makes each one urgent, and what treatment actually involves helps you respond appropriately when you spot one.
At the Veterinary Emergency and Specialty Center of Northern Arizona, abscesses of all types are part of what we evaluate and treat. Whether the presentation is a bite wound that festered over a few days or a deep facial infection requiring imaging and surgery, our team has the diagnostic capability and the surgical expertise to address it. We are open for emergency care from 5 p.m. Friday through 8 a.m. Monday, which means around-the-clock coverage through the weekend when most practices are closed. Call us or come in directly during our open hours if your pet has unexplained swelling, pain, or wound drainage.
What an Abscess Is and How One Forms
An abscess is a walled-off pocket of infection filled with pus, formed when the body tries to contain bacteria that have invaded tissue. When bacteria enter through a wound, a diseased tooth, or a puncture, the immune system responds by sending white blood cells to fight the infection. If the infection cannot be fully cleared, the body walls it off, and the resulting pocket of cellular debris and bacteria grows under pressure.
Abscesses can form almost anywhere. Some are superficial and visible: a soft, warm lump under the skin that becomes obvious within days. Others are deep and produce very few local signs, instead presenting as systemic illness: fever, lethargy, and reduced appetite with no obvious external cause. Regardless of where an abscess forms, the underlying principle is the same: it will not resolve on its own, and drainage alone without addressing the cause and providing antibiotics is not adequate treatment.
Cytology and sampling with biopsy are important diagnostic tools that help distinguish abscesses from other causes of swelling, including tumors and cysts, which can look similar on the surface.
General Signs of an Abscess
Across all types and locations, abscesses tend to produce some combination of:
- Localized swelling that may feel soft and fluctuant or firm
- Warmth and pain at the site
- Discharge or drainage, which may appear suddenly when an abscess ruptures
- Fever
- Lethargy and reduced appetite
- Common pet pain signs including guarding, reluctance to move, limping, or change in posture
Deep abscesses, particularly internal or retrobulbar infections, may produce very few visible local signs while causing significant systemic illness. Any unexplained change in your pet’s energy, appetite, or behavior alongside any new swelling is worth evaluating the same day rather than watching at home. Contact us or come in directly during our open hours.
Bite Wound Abscesses
Bite wound abscesses are among the most common abscess presentations in cats with outdoor access. Cat bites create deep, narrow puncture wounds that seal over at the surface within hours while bacteria are driven deep into the tissue, where they proliferate in a warm environment perfectly suited for abscess formation.
Bite wounds in cats are often discovered only after an abscess has already developed, because punctures through a thick coat are easy to miss. A cat abscess typically becomes apparent 3 to 5 days after the fight: a warm, painful swelling, often on the face, neck, tail base, or limbs, that may rupture and drain foul-smelling fluid. Bite wound abscesses also occur in dogs, so any puncture wound should be treated promptly regardless of species.
If you witnessed the fight, apply light pressure to any bleeding wound and seek emergency care for your pet promptly rather than waiting for signs of infection. Early treatment before an abscess develops requires only antibiotics and wound cleaning. Waiting until an abscess has formed means lab work, anesthesia, surgical debridement of the abscess and possible drain placement, and longer courses of antibiotics and pain medications.
Complications of Delayed Treatment
Bite wound abscesses that are not treated promptly can extend into deeper tissue planes, affect underlying joints or bones, or progress to septic shock. Even an abscess that appears to have drained on its own still requires veterinary evaluation, as surface drainage does not clear the deep infection and the drain hole often re-seals and fills back up. At VESCONA, our bite and wound care capabilities handle the full range from simple abscesses to complex deep infections.
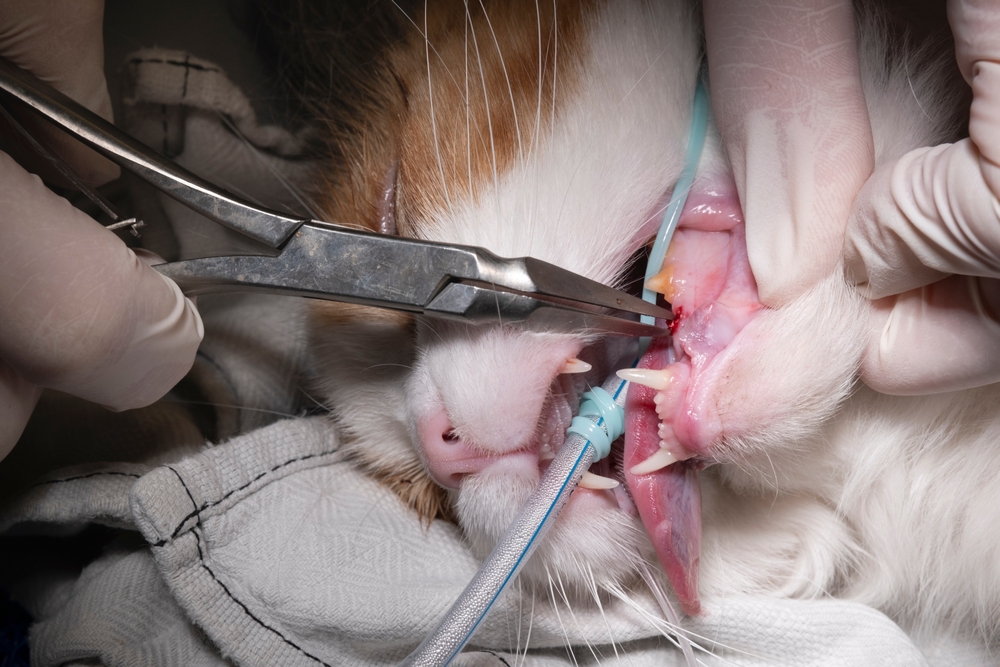
Tooth Root Abscesses
Tooth root abscesses develop at the tip of a tooth’s root when untreated periodontal disease, a fractured tooth, or trauma allows bacteria to invade the root canal and surrounding bone. Because the abscess forms below the gum line, it is invisible without dental X-rays until it becomes so large that it swells and ruptures through the skin. The problem is often noticed only when facial swelling or behavior changes prompt a closer look.
In dogs, the carnassial tooth (the large upper fourth premolar) is one of the most commonly affected, often in dogs that chew aggressively and have broken off the outer enamel of the tooth. An abscess here typically produces swelling just below the eye or sometimes behind the eye, called a retrobulbar abscess.
Retrobulbar Abscesses
Retrobulbar abscesses produce a distinctive cluster of signs: one eye protruding more than the other, obvious pain when the mouth is opened, swelling or a soft fluctuant mass behind the last upper molar visible from inside the mouth, and fever. Penetrating mouth wounds and foreign bodies can also be responsible, like from sticks, foxtails, toothpicks, or skewers.
Complications of Untreated Dental and Retrobulbar Abscesses
Dental abscesses left untreated erode through surrounding structures. They can break into the nasal passages creating oronasal fistulas with chronic one-sided nasal discharge, damage the eye, or allow bacteria to spread systemically and affect the heart, kidneys, and liver. Treatment requires extraction of the affected tooth and thorough debridement of the infected site.
Anal Gland Abscesses
Anal glands are small scent-producing sacs located on either side of the rectum. When their secretions thicken and fail to empty normally, they become impacted. Untreated impaction progresses to infection and abscess formation. A ruptured anal gland abscess produces a visible, painful wound adjacent to the anus that looks alarming but responds well to treatment when addressed promptly.
Signs of impaction before rupture include scooting, licking or biting at the tail base, difficulty sitting, foul odor, and visible swelling. Expressing anal glands at the appropriate interval manages impaction, but timing varies significantly by individual. Anal gland ruptures often require sedation or anesthesia for flushing of the gland, instilling a medication into the ruptured site, and pain medications plus antibiotics to go home. Anal sac diseases that are recurrent or severe sometimes require surgical removal of the glands entirely.
Why Anal Gland Problems Recur
Anal gland impaction frequently recurs in pets with underlying allergies or skin inflammation that affects gland consistency. In rare cases, recurrent anal gland disease is driven by anal sac adenocarcinoma, which should be ruled out in any dog with severe, recurrent, or treatment-resistant disease.
Foxtails and Plant Awn Abscesses
Few things in the northern Arizona landscape cause as many abscesses as foxtails and other grass awns. Foxtails are the barbed seed heads of several grass species that thrive in dry, open areas across our region, and they are engineered by nature to move in only one direction: forward. Once an awn lodges in fur or skin, every movement drives it deeper. It does not come out on its own, and it does not break down inside the body.
The problem is that foxtails can enter almost anywhere, and carry bacteria with them. Common entry points include between the toes, inside the ears, under the eyelids, up the nose, and into the skin along the belly, chest, or armpits. Once embedded, the awn migrates through tissue, creating an infection tract as it goes. The outward result is often a non-healing draining wound, a soft fluctuant swelling, or a recurring abscess that seems to “come back” each time it is drained because the underlying foreign body was never removed.
Foxtail abscesses are among the cases that reinforce why antibiotics alone are not adequate treatment. The foreign body must be located and removed, often through imaging followed by surgical exploration, before the infection can truly clear. Our diagnostic imaging capability with CT scanning is particularly valuable for foxtail cases, where the seed head has often migrated far from the original entry point by the time the abscess is found.
Valley Fever and Abscesses
Valley Fever is a fungal infection caused by Coccidioides organisms that live in the soil throughout Arizona. Dogs become infected by inhaling fungal spores kicked up from disturbed soil, which is nearly impossible to avoid in our dry, dusty environment.
Most Valley Fever cases start in the lungs with signs like coughing, lethargy, reduced appetite, and weight loss. In some dogs, though, the infection spreads beyond the lungs and settles in other tissues, including the bones, skin, and lymph nodes. When it localizes in these deeper tissues, the result can look remarkably like an abscess: a firm, painful swelling, sometimes with a draining tract at the skin surface that refuses to heal despite antibiotics.
Valley Fever lesions are often mistaken for routine bite-wound abscesses or foxtail tracts at first glance, which is why diagnostics matter so much in this region. Diagnosing Valley Fever requires blood testing (the Valley Fever titer) and often imaging to evaluate the lungs and bones for additional involvement. Cytology or biopsy of the lesion itself sometimes shows the distinctive fungal organisms, which is how the diagnosis gets confirmed in some cases.
Treatment is completely different from treating a bacterial abscess. Valley Fever treatment requires months of oral antifungal medication, typically fluconazole or itraconazole, and many dogs need a year or more of therapy to fully clear the infection. Some cases require lifelong treatment when the fungus cannot be fully eradicated. Simply lancing and flushing a Valley Fever lesion as if it were a bacterial abscess will not resolve the underlying infection, and the swelling will return. This is one of the most important reasons to bring any non-healing wound or recurring abscess in for evaluation rather than treating it at home or assuming antibiotics alone will handle it.
Other Abscess Types
Subcutaneous foreign body abscesses: Beyond foxtails, other plant debris, wood splinters, and thorns in northern Arizona can penetrate the skin and track deep into tissue, creating infection pockets that require surgical foreign material removal alongside antibiotics. Antibiotics alone rarely resolve these cases.
Internal abscesses: Prostatic abscesses, abdominal infections, and organ-adjacent infections present as systemic illness with abdominal pain or vague lethargy. These require imaging for diagnosis and often surgical drainage.
Interdigital furuncles (paw abscesses): Painful nodules between the toes, common in dogs with allergies or anatomical factors that trap moisture in the paws. Frequently recurrent without addressing the underlying cause.
How Abscesses Are Treated
Treatment principles apply across all types: the infection must be drained, the underlying cause must be addressed, and antibiotic therapy is required.
Treatment options by severity:
- Lance and flush: for accessible, mature superficial abscesses; performed under sedation or local anesthesia
- Surgical debridement: for deeper infections, necrotic tissue, or foreign bodies requiring removal
- Drain placement: for larger cavities requiring continued drainage during healing
- Tooth extraction: for dental abscesses; the infected tooth cannot be retained
- Anal gland removal: for recurrent or severe anal gland disease unresponsive to conservative management
- Hospitalization and IV antibiotics or antifungals: for pets with systemic illness, sepsis risk, or inability to eat
Pain management is part of every treatment plan. Abscesses are painful, and comfort during and after treatment is not optional. Follow-up to confirm healing and appropriate antibiotic response is always scheduled. For recurrent abscesses, imaging including a CT scan to look for foreign objects and culture to find the correct type of medication is warranted.
Frequently Asked Questions
Can I treat an abscess at home?
No. Abscesses require veterinary drainage and systemic antibiotics to resolve. Home management of a draining abscess without treatment delays care and allows the infection to deepen.
My cat’s abscess burst on its own. Does it still need treatment?
Yes. Surface drainage does not clear the deep infection. A ruptured abscess still requires flushing, assessment of the wound, and antibiotic therapy to prevent re-formation and systemic spread.
How long does an abscess take to heal after treatment?
Most simple superficial abscesses heal within 1 to 2 weeks with appropriate treatment. Deeper infections, foreign body abscesses, or dental abscesses requiring surgery have longer recovery timelines.
Will my pet need surgery?
Many abscesses can be drained and flushed without general surgery. Dental abscesses always require tooth extraction. Foxtails and other foreign bodies require surgical removal. Retrobulbar and deep tissue abscesses often require surgical drainage. Your pet’s specific presentation determines the approach.
How do I know if a lump is an abscess or something else?
Pain, warmth, and rapid appearance suggest infection. Firm, painless lumps that have been present for weeks without change suggest a non-infectious cause. The only reliable way to distinguish between these is veterinary evaluation and sample collection.
When Swelling Appears, Act Promptly
Abscesses are common, always painful, and almost always require more than time to resolve. The good news is that most pets respond very well to appropriate treatment and recover fully when care is sought before the infection deepens.
VESCONA is open for weekend emergency care from 5 p.m. Friday through 8 a.m. Monday and handles complex abscesses in-house with comprehensive diagnostic imaging and surgical care. Contact us or come directly to our Flagstaff facility during our open hours. Our team is ready to help.






Leave A Comment