Auto-Immune Blood Diseases: What’s Happening and Why Emergency Care Matters
Few moments are scarier than watching your pet go from “a bit off” to clearly very sick in the space of an afternoon. With auto-immune blood diseases, that’s often exactly how it plays out. Conditions like immune-mediated hemolytic anemia and immune-mediated thrombocytopenia happen when your pet’s immune system, which is supposed to be defending against germs and threats, accidentally turns its weapons on the body’s own blood cells. The destruction can happen faster than the body can keep up with, and pets can go downhill alarmingly quickly.
The good news: when caught early and treated aggressively, many of these pets pull through and go on to do well. The challenge is recognizing the signs in time and getting to a hospital that can act fast.
That’s where we come in. The Veterinary Emergency and Specialty Center of Northern Arizona in Flagstaff has the diagnostics, critical care capabilities, and experienced emergency team needed to handle these cases under one roof. When a pet arrives in crisis, having the right tools immediately available is what makes the difference. If your pet is suddenly weak, has pale gums, or is bleeding or bruising in ways that don’t make sense, contact us or come straight to our facility.
Why Does the Immune System Sometimes Attack the Blood?
The immune system is supposed to recognize the difference between “foreign invader” and “this is part of me, leave it alone.” Sometimes it loses that ability. With immune-mediated diseases, the immune system mistakenly tags red blood cells or platelets as threats and starts destroying them.
The fallout depends on which cells are under attack:
- When red blood cells are destroyed faster than the body can replace them, oxygen delivery to organs starts failing. Your pet becomes weak, pale, and short of breath.
- When platelets are removed from circulation, the blood loses its ability to form clots. Even small blood vessel injuries that would normally heal on their own can keep bleeding.
Sometimes there’s no clear reason the immune system goes haywire (this is called primary or idiopathic disease). Other times, something specific kicks the immune system into overdrive- an infection, a tumor, a toxin, or another underlying health problem (this is called secondary disease). Telling these apart matters a lot for treatment.
| Primary Disease | Secondary Disease |
| No identifiable trigger | A specific cause is driving the immune attack |
| Treated with immunosuppression alone | Must address both the immune attack AND the underlying cause |
| Common triggers include infections, cancer, toxins, or other diseases | |
| Treating without addressing the trigger leads to incomplete recovery and frequent relapse |
Sorting out which type your pet has shapes everything that comes next.
IMHA in Dogs and Cats
Immune-mediated hemolytic anemia (IMHA for short) is one of the most common and most serious immune-mediated conditions in dogs. It happens in cats too, just less often. Red blood cells are getting destroyed, oxygen delivery falls behind, and the body works overtime to make new red blood cells fast enough to keep up.
Some pets show up with mild symptoms, looking a little tired and not quite themselves. Others arrive in full crisis, barely able to stand. The frightening part is how quickly the picture can change. A pet who seems mildly off in the morning can be in serious trouble by evening.
How Do You Recognize Early Signs of IMHA?
The earliest signs are subtle, but recognizable when you know what to look for:
- Unusual fatigue or exercise intolerance that wasn’t there a week ago
- Faster breathing at rest, as the body tries to compensate for less oxygen reaching the tissues
- Pale or yellow gums: as red blood cells break down, a yellow tinge can develop in the gums, eyes, or skin
- Dark, orange, or red-tinged urine from the breakdown products of destroyed red blood cells
- Decreased appetite
- A racing heart at rest, which you might notice as a pulse that feels much faster than usual
- Weakness or reluctance to do walks they’d normally enjoy
- Collapse in advanced cases
Some breeds are more likely to develop IMHA than others. Cocker Spaniels, English Springer Spaniels, Old English Sheepdogs, and Poodles all have documented breed predispositions. If your dog is in this group, it’s worth being a little extra alert when you notice them slowing down for no obvious reason.
What Triggers Secondary IMHA?
When IMHA is secondary to something else, finding the trigger is part of getting your pet better. Common culprits include:
- Tick-borne infections like Ehrlichia, Anaplasma, Babesia, and Rocky Mountain spotted fever, all of which can kick off IMHA in dogs with tick exposure
- Leptospirosis, picked up through contact with contaminated water or wildlife urine. Lepto is a real concern for dogs who play in puddles, ponds, or rural areas
- Hemotropic mycoplasma in cats, particularly outdoor cats or cats with a history of fight wounds. This infection directly attacks red blood cells and can also trigger an immune response
- Cancer, including lymphoma and hemangiosarcoma
- Toxins like zinc, which can come from swallowed pennies, hardware, or zinc oxide creams
- Certain medications, and even snake bites in some cases
The Clotting Problem in IMHA
Here’s something that catches families off guard: while red blood cells are being destroyed and your pet is becoming severely anemic, the clotting system can simultaneously go haywire in a different direction, forming abnormal clots where they shouldn’t be.
IMHA patients are at high risk for clots traveling to the lungs (called pulmonary thromboembolism), and these clots are one of the leading causes of death in IMHA cases. Signs that a clot may have formed and need immediate evaluation:
- Sudden labored breathing
- Coughing or coughing up blood
- Sudden inability to use a leg
- Collapse
- Acute changes in alertness or mental state
This is one of the main reasons newly-diagnosed IMHA patients need to be hospitalized rather than treated as outpatients, especially during the first 1 to 2 weeks. Continuous monitoring catches these complications early when there’s still time to do something about them.
ITP in Dogs and Cats
Immune-mediated thrombocytopenia (ITP) is the platelet version of the same problem. Platelets are tiny cell fragments that plug small leaks in blood vessels and form the foundation for clotting. When the immune system destroys them, your pet loses the ability to stop bleeding properly.
The tricky thing about ITP is that internal bleeding can be much worse than what you can see on the outside. Your dog with a few small purple spots on the gums and mild lethargy might also be bleeding into the GI tract, urinary system, or even the brain.
Recognizing Signs of ITP in Pets
What to look for:
- Unexplained bruising on the belly, gums, or other areas without any known injury
- Petechiae: pinpoint purple-red spots, especially on the gums, belly, and inside of the ear flaps
- Nosebleeds with no trauma
- Blood in the urine or stool
- Wounds that keep bleeding longer than they should
- Pale gums if your pet has been losing blood internally
- Lethargy and weakness
What Can Trigger ITP in Dogs and Cats?
The triggers overlap a lot with IMHA:
- Tick-borne infections, especially Ehrlichia, Anaplasma, and Rickettsial diseases
- Heartworm disease
- Distemper virus in unvaccinated dogs
- Leptospirosis
- Certain medications
- Cancers like lymphoma
Recent vaccination has been linked to ITP in rare cases. The benefits of vaccination far outweigh that small risk, but if your pet was recently vaccinated and develops bleeding signs, your vet will want to know.
Evans Syndrome in Pets
When the immune system goes after both red blood cells and platelets at the same time, it’s called Evans syndrome. These pets have both IMHA and ITP simultaneously, which combines both sets of problems. Treatment has to address both, and the prognosis is generally tougher than for either condition alone.
Tick-Borne Diseases and Immune-Mediated Blood Disorders
The tick connection deserves its own moment because tick-borne infections can either trigger immune-mediated blood disease or look almost exactly like it. If a vet treats apparent primary disease without ruling out a hidden tick-borne infection, the case often comes back, sometimes worse than before.
| Tick-Borne Infection | What It Causes |
| Lyme disease | Immune-mediated complications including thrombocytopenia, joint disease, and kidney problems |
| Rocky Mountain spotted fever | Acute illness with fever, low platelets, and various organ effects (despite the name, it occurs across much of North America) |
| Ehrlichia and Anaplasma | Low platelets are common, and these infections can drive concurrent immune-mediated processes |
| Babesia species | Direct red blood cell destruction and can also kick off an immune-mediated component |
Tick-borne disease testing is a standard part of any IMHA or ITP workup, even when families don’t think their pet has been exposed. Some of these infections can sit quietly for months before causing trouble.
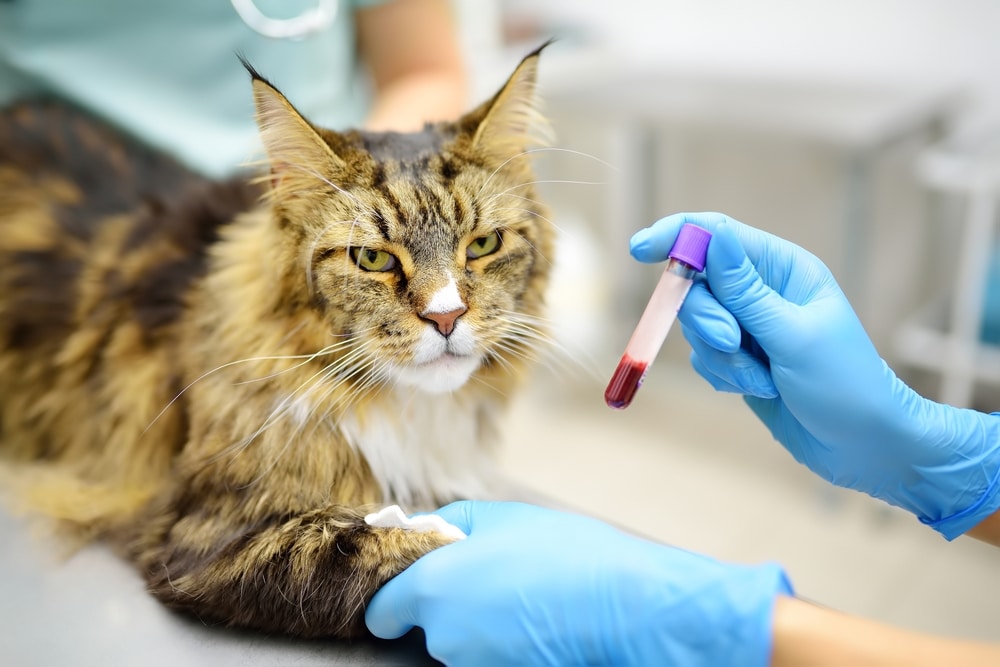
How Are Immune-Mediated Blood Diseases Diagnosed?
Diagnosis starts with the conversation in the exam room and your pet’s physical exam, then moves quickly to specific testing. We’ll ask you about recent illnesses, medications, vaccines, travel, tick exposure, and anything your pet might have gotten into. The physical exam looks for signs of anemia or bleeding and any clues pointing toward an underlying cause.
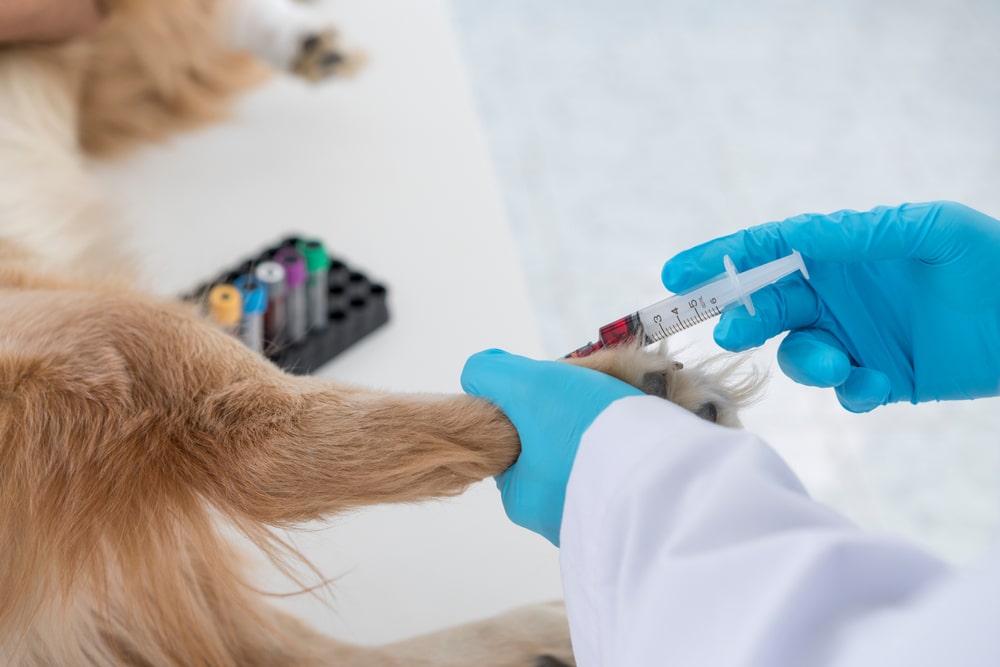
The diagnostic test panel typically includes:
- Complete blood count with reticulocyte count to evaluate the bone marrow’s response
- Blood smear examination to look for telltale signs like spherocytes (a hallmark of IMHA), platelet clumps, blood parasites, and other findings
- Coombs test to detect antibodies attached to red blood cells
- Chemistry panel to evaluate organ function and look for triggers
- Urinalysis to check for hemoglobin in the urine, evaluate kidney function, and screen for leptospirosis
- Tick-borne disease screening as a routine part of the workup
- Imaging (X-rays and ultrasound) to look for hidden cancer, organ enlargement, or other issues
- Bone marrow evaluation in select cases
Our in-house lab capabilities mean many of these results come back the same visit, which is critical when your pet can’t wait.
Treating IMHA and ITP in Dogs and Cats
Treatment has two parallel goals: stop the immune attack, and support the body while blood counts recover. When there’s a secondary trigger, treating that becomes the third critical piece.
IMHA Treatment
- Immunosuppression with corticosteroids (typically prednisone) as the first-line treatment, with additional immunosuppressive medications added for moderate to severe cases
- Anti-clotting medications for high-risk patients to head off those dangerous lung clots
- Supportive care including IV fluids, oxygen support, and continuous monitoring
- Blood transfusions for severely anemic patients to keep oxygen delivery going while the immunosuppression takes effect
- Therapeutic plasma exchange for severe cases that aren’t responding. This advanced approach actually filters antibodies out of the bloodstream, and blood purification techniques have produced dramatic turnarounds in cases that weren’t responding to standard therapy
- Targeted antibiotics or antiparasitics when an infectious trigger is found
Treatment runs over months, not weeks. The intensive phase usually lasts 1 to 2 weeks, then medications are gradually tapered over 3 to 6 months as your pet stabilizes. Tapering too fast is one of the most common reasons cases relapse, so patience here matters.
ITP Treatment
- Corticosteroids as first-line therapy, often at higher initial doses than for IMHA
- Vincristine, a single dose that helps boost platelet release from the spleen and bone marrow
- Intravenous immunoglobulin (IVIG) for the most critically low platelet counts or active bleeding
- Additional immunosuppressants for cases that need more than corticosteroids alone
- Splenectomy (surgical removal of the spleen) as a later option for cases that haven’t responded to medical therapy
- Blood product transfusions if bleeding has caused significant anemia
While platelet counts are dangerously low, your pet needs careful handling. Soft food, no rough play, no procedures that could cause bleeding, and gentle handling all matter during this window.
What Warning Signs Call for Urgent Veterinary Attention?
These signs warrant same-day evaluation. If you notice any of them in your pet, contact us or come straight to our emergency facility:
- Sudden weakness, collapse, or inability to stand
- Pale, white, or yellow gums
- Unexplained bruising or pinpoint red spots on the gums, belly, or other areas
- Labored breathing at rest or noticeably increased breathing effort
- Dark, orange, red, or blood-tinged urine
- Significant lethargy or unresponsiveness
- Nosebleeds without injury
- Vomit or stool with blood
- Wounds that bleed longer than expected
Calling ahead lets our team prepare for your arrival and have the right resources ready. The minutes saved can matter substantially in the most critical cases.
Frequently Asked Questions About IMHA and ITP in Pets
How quickly can these conditions become life-threatening?
Fast. Some pets deteriorate over a few days, others can go from mild signs to a true crisis in hours. That’s why same-day evaluation matters so much when warning signs show up.
Will my pet be on medications for life?
Most pets need treatment for at least several months. Some can eventually be tapered off all medications and stay in remission. Others need a low maintenance dose for life. Your vet will work out the right plan based on how your specific pet responds.
What’s the prognosis?
It depends on how severe things are when treatment starts, how well your pet responds, and whether any underlying triggers can be identified and addressed. With prompt diagnosis and aggressive treatment, many pets do well. Cases that develop complications like lung clots, or that don’t respond to standard therapy, are tougher.
Can these conditions come back?
Yes, unfortunately. Finding and treating any underlying triggers reduces relapse risk substantially. Tapering immunosuppressants too quickly is one of the most common ways relapses happen, which is why these treatments take months to wind down.
Moving from Uncertainty to a Treatment Plan
When your pet arrives at our hospital suddenly weak, pale, or bleeding, everything moves fast and it can be overwhelming for a family to keep up. The reassuring counterweight: when these conditions are caught quickly and treated aggressively, many pets pull through. The pets who do best are the ones whose families recognized that something was wrong and acted on it.
If your pet is showing any of the warning signs, contact us at the Veterinary Emergency and Specialty Center of Northern Arizona. Our team is here 24/7 every weekend, ready to evaluate, diagnose, and start treatment.






Leave A Comment